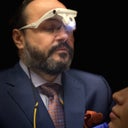
Is this breast tissue necrosis or just a scab? (photo)
I saw my PS on Monday and he stated he wanted to see me again in two weeks for this "scab?" After a little research on this site, it appears as if this may be more than a scab. Seems to me like it is Necrosis. Any opinions would be helpful, and also, what kind of treatment is usually used for situations like this? Should I wait two weeks or is this something that needs to be addressed ASAP. As of right now, he has advised me to do nothing until I see him again in two weeks.